For pregnant women, routine visits to the OB-GYN can be emotional. The list of things that can go wrong during pregnancy seems endless, and women rely on their doctors to catch and treat anything that could prevent a healthy delivery. One of those conditions is pre-eclampsia, which occurs in 3 to 7 percent of all pregnancies. Talking to a Pre-Eclampsia lawyer can help review your situation.
Pre-eclampsia is characterized by high blood pressure and protein in the mother’s urine. Generally, the only effective treatment for pre-eclampsia is delivering the baby. However, a mother may have a pre-eclampsia malpractice claim if her doctor failed to diagnose or manage the condition. If you suffered from pre-eclampsia and your doctor should have caught the condition, an experienced lawyer can help you receive the compensation to which you are entitled. Attorney Janet Izzo is the founding attorney at Izzo Law Office, and she represents women in Syracuse and throughout New York who were victims of birth injuries and OB-GYN malpractice.
From a Preeclampsia Lawyer: A Serious Pregnancy Complication
Preeclampsia is a pregnancy-specific condition characterized by high blood pressure and signs of organ damage, most commonly affecting the liver and kidneys. This disorder typically develops after the 20th week of pregnancy in women whose blood pressure was previously normal, though it can occasionally appear earlier or even during the postpartum period up to six weeks after delivery.
The exact cause of preeclampsia is not fully understood, but it is believed to originate with problems in the placenta—the organ that develops during pregnancy to provide oxygen and nutrients to your baby. When blood vessels supplying the placenta don’t develop properly, blood flow becomes restricted. This triggers a cascade of problems, including high blood pressure in the mother and inadequate blood supply to the baby.
Signs and Symptoms of Preeclampsia
The March of Dimes provides a great review of signs and symptoms:
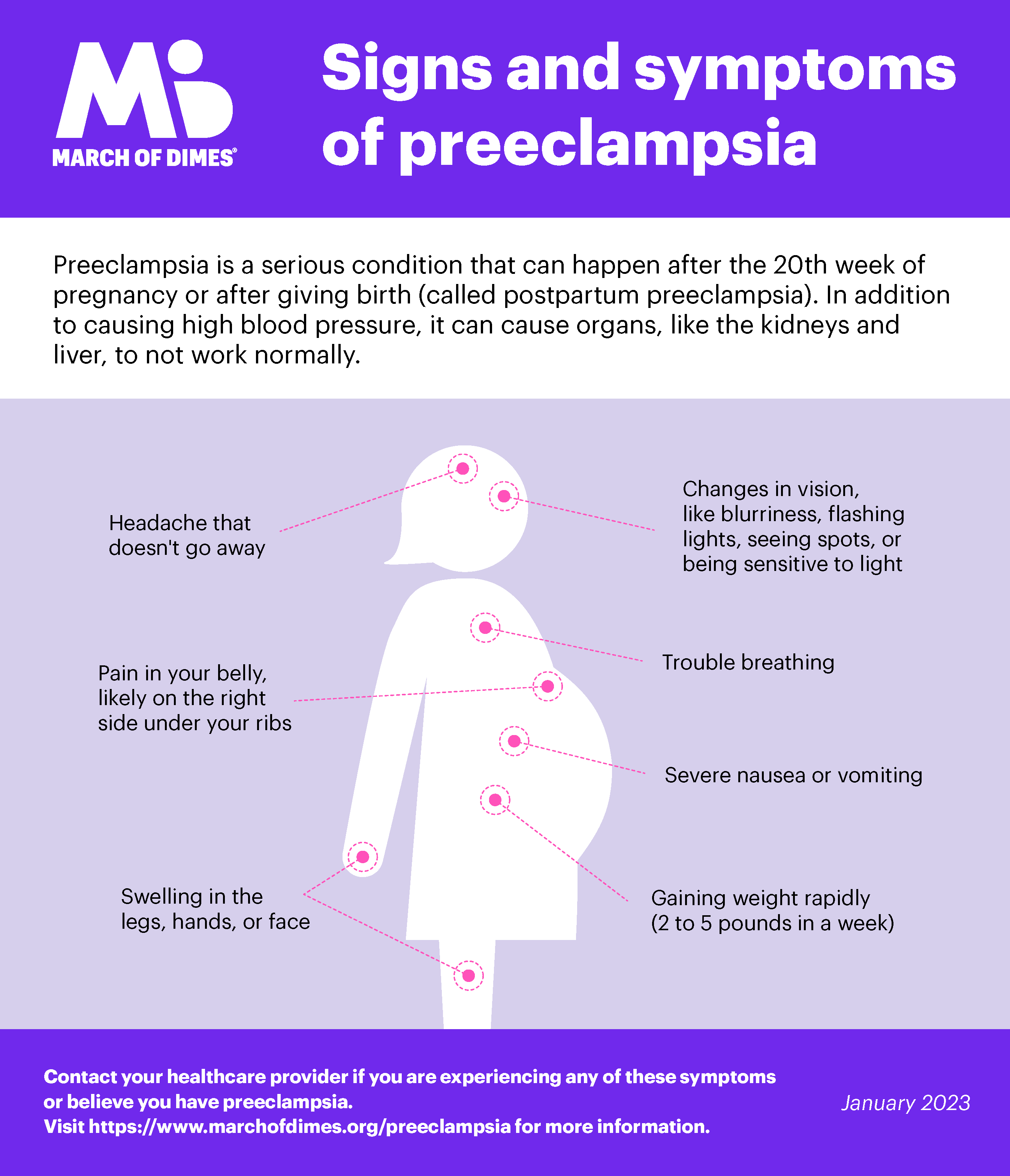
Preeclampsia often develops gradually, but it can also appear suddenly and progress rapidly. Many women feel fine and have no symptoms, which is why regular prenatal monitoring is essential. When symptoms do occur, they may include:
High blood pressure is the hallmark sign, defined as a reading of 140/90 mm Hg or higher on two occasions at least four hours apart. Severely elevated blood pressure (160/110 mm Hg or higher) indicates severe preeclampsia requiring immediate intervention.
Proteinuria, or excess protein in the urine, indicates that preeclampsia is affecting kidney function. This is detected through urine tests during prenatal visits. Protein levels of 300 mg or more in a 24-hour urine collection or a protein-to-creatinine ratio of 0.3 or higher indicates significant kidney involvement.
Severe headaches that don’t respond to over-the-counter pain medication and persist despite rest can indicate that preeclampsia is affecting your brain and increasing intracranial pressure.
Vision changes, including blurred vision, seeing spots or flashing lights, light sensitivity, or temporary vision loss occur when preeclampsia affects the blood vessels in your eyes or the visual processing areas of your brain.
Upper abdominal pain, particularly under the ribs on the right side, indicates that preeclampsia is affecting your liver. This pain is often severe and may be accompanied by nausea.
Shortness of breath can occur when fluid accumulates in the lungs due to preeclampsia’s effects on blood vessels and organ function.
Sudden weight gain and swelling (edema), particularly in the face and hands, results from fluid retention. While some swelling is normal during pregnancy, sudden and severe swelling is concerning.
Decreased urine output indicates worsening kidney function and suggests preeclampsia may be progressing to a more severe stage.
It’s important to understand that preeclampsia can be dangerous even without obvious symptoms. This is precisely why healthcare providers must diligently monitor blood pressure and perform urine tests at every prenatal visit.
Risk Factors for Developing Preeclampsia
While preeclampsia can affect any pregnant woman, certain factors increase your risk:
-
First pregnancy: Women who are pregnant for the first time face higher risk.
-
Previous preeclampsia: Having had preeclampsia in a prior pregnancy significantly increases the likelihood of recurrence.
-
Maternal age: Women over 35 or teenage mothers have elevated risk.
-
Obesity: Having a body mass index (BMI) of 30 or higher increases risk.
-
Multiple pregnancy: Carrying twins, triplets, or more multiples increases risk.
-
Pre-existing conditions: Chronic high blood pressure, diabetes, kidney disease, lupus, and other autoimmune disorders increase susceptibility.
-
Family history: Having a mother or sister who had preeclampsia increases your risk.
-
In vitro fertilization (IVF): Pregnancies resulting from IVF have higher preeclampsia rates.
-
Interval between pregnancies: Waiting 10 or more years between pregnancies increases risk.
Healthcare providers have a duty to identify women at high risk for preeclampsia and monitor them more closely throughout pregnancy. They should also prescribe low-dose aspirin for high-risk women, as research shows this can reduce the incidence of preeclampsia when started between 12 and 28 weeks of pregnancy.
Protect Your Family; Talk To A Pre-Eclampsia Lawyer Today
If you were the victim of untreated or misdiagnosed pre-eclampsia, contact Gillette & Izzo Law Office to schedule a free initial consultation with an experienced lawyer. Complete our online contact form or call 315-421-1000 to schedule your consultation.
We handle all birth injury cases on a contingency basis, which requires no payment upfront, and you only pay us if we successfully recover on your behalf.
